Fitting ICD FlexFit with the Medmont meridia
Streamlining your scleral fitting process is possible with help from the Medmont meridia.
A case for diagnostic fitting
Despite the recent advancements in anterior segment imaging technology, the hurdle that presently plagues all imaging systems that offer empirical scleral lens design and fitting is the matter of lens power. While the relationship of corneal curvature and manifest refraction to final contact lens power is very predictable in the normal eye, all bets are off when it comes to the irregular cornea. Manifest refraction, and even retinoscopy, on those with irregular corneas often yield questionable results at best and lead practitioners down a vortex of wasted chair time at worst.
That’s why placing a diagnostic lens on the eye continues to be a critical step in the overall scleral fitting process. By masking the irregular corneal surface with a diagnostic lens that has a smooth, consistent refractive surface, the over-refraction process suddenly becomes much easier and faster. An accurate first lens power ensures patients experience the “wow” factor of clear vision when the lenses are first applied. Correct initial lens power also reduces the number of lens remakes. Plus, you get the opportunity to see how the lens is actually fitting, not just a theoretical model of how a lens should fit.
Making diagnostic lens selection a no-brainer
If the diagnostic scleral fitting set isn’t going the way of the rotary phone, how do we maximize its efficiency? By ensuring the first ICD FlexFIt diagnostic lens selected will provide the best initial fit. By selecting a lens that is within +/-150 microns of the final desired central clearance value, your chance of determining an accurate first lens power is maximized. Following ICD FlexFIt’s straightforward lens selection guide based on corneal condition will get you to the right lens the majority of the time. But, there are times when certain diseased eyes require a different diagnostic lens than expected. Cases like these highlight the value of using instruments like the medmont meridia to confirm our assumptions about the ocular surface sagittal height values for particular patients. It’s quick, easy, and really comes down to a simple 3 step process.
Step 1: Capture quality topography
The speed and ease with which the meridia captures topography images is one of its stand out benefits. There is no need for repeatedly instilling fluorescein throughout the capture process. An adequate and stable tear film is all that is required for a quality capture, so a stash of preservative free artificial tears on the instrument table is nice to have. The composite map feature of the medmont system allows the entire cornea to be imaged accurately and precisely. With a little training on the “tips and tricks” of captures and a little practice, this is something a technician can often perform in 5 minutes or less.
At this point, the question, “why do we need a quality corneal topography capture when fitting a lens that doesn’t touch the cornea?” inevitably comes up. While it’s true that information about the central cornea may not be particularly helpful, accurate peripheral cornea data are the critical pieces the Medmont system uses to estimate the eye height at different chords. The consistent nature of the sclera-corneal angle allows for surprisingly accurate eye height estimates at chord lengths of up to 18 mm. When a quality composite map is captured with the medmont, it has been shown to provide similar results about eye height compared to common anterior segment OCT imaging systems.
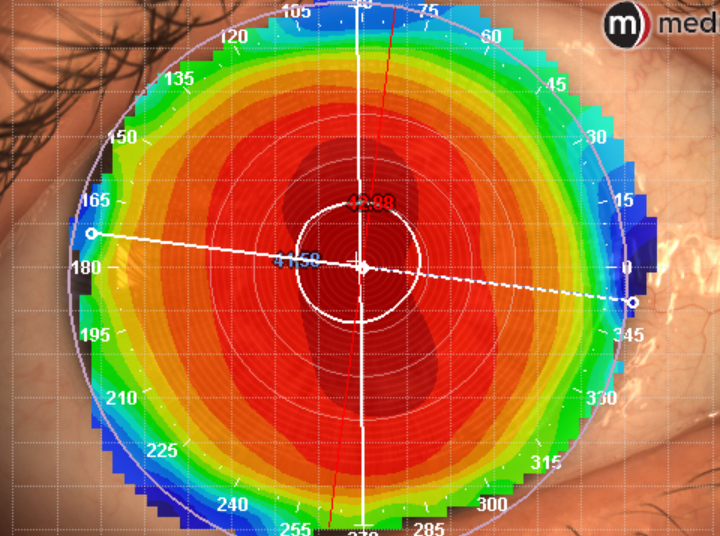
Step 2: Select diagnostic lens based on desired diameter and Eye Height at the corresponding cord
Once a quality composite topography has been captured, the hard work is done. The diameter of the lens can be determined by the HVID (another easy piece of information to gather from the medmont), corneal condition, or other characteristics of the patient (narrow fissures for example). The diameter of the lens is simply entered into the medmont software and the approximate eye height at that chord length will be given. All that’s left to do is grab the diagnostic lens closest to the estimated height given.

In the example above, the 16.5 mm, 4200 SAG ICD FlexFIt lens would be used. Again, this is something a technician can do.
Step 3: Place lens on eye
All that’s left is to apply the diagnostic lens then evaluate fit and over-refract. As you may have guessed, a technician can apply the lenses.
Wrapping things up
The time it takes technician team members to capture topography images, select the correct diagnostic lens, and apply the lens is approximately 12-15 minutes. You may consider adding a quick trip to the auto-refractor to get a starting point for the critical over-refraction. That way, the doctor’s responsibilities only involve a detailed evaluation of the lens fit and a simple refinement of lens power. But even in its current state without the auto-refractor step, only about 10 minutes of doctor time is required.
Whether you’re a seasoned ICD FlexFIt lens fitter or looking to get started, the ICD FlexFit fitting with medmont can help simplify and speed up the process. That means you get to spend more time building trust and confidence with your patient and less time removing and applying various diagnostic lenses in those cases where the initial diagnostic lens suggested based on corneal condition isn’t quite right.
Bonus features
Don’t forget Medmont remains the top choice for ortho k fitters because of its accuracy and precision. Other scleral profilometry units often sacrifice topography quality in favor of other features. The Pro model also has state-of-the-art dry eye diagnostics and anterior segment imaging features. A quick capture of the scleral lens with the meridia can help the knowledgeable consultants at Precision and Cardinal assist you with any fit changes that need to be made. They can also help start the process of making the Medmont meridia a part of your practice.
Contact them at consultation@ptsoptics.com or consultation@cardinalcontactlens.com to learn more about ICD FlexFit Fitting with Medmont topographers.
